What Does Level 5 Services Mean Csii?
This memo serves four purposes: (ane) outlines the description and treatment of diabetes mellitus; (2) reviews the history of Medicare's coverage policies on diabetes management; (3) analyzes the relevant scientific data related to the continuous subcutaneous insulin infusion (CSII) pump; (4) delineates the reasons supporting a positive national decision to comprehend the device for type I diabetics. A. Pathophysiology Diabetes Mellitus is a affliction of abnormal glucose metabolism characterized by a deficiency of insulin production, or by evolution of insulin-resistance, either of which results in abnormally high blood sugars. Diabetes Mellitus is mostly subdivided into two categories: (ane) Type I diabetes mellitus , (likewise known as insulin dependent diabetes mellitus [IDDM] or juvenile onset diabetes mellitus) and (2) Blazon Ii diabetes mellitus (also known as non insulin dependent diabetes mellitus [NIDDM] or adult onset diabetes mellitus)1 Blazon I diabetes may begin at any age but onset typically occurs in childhood or adolescence. Type I diabetes results from an allowed mediated devastation of pancreatic islet beta cells causing decreased endogenous secretion of insulin and necessitating exogenous insulin therapy to maintain euglycemia. Blazon II diabetes is marked past peripheral resistance to the effect of insulin rather than absolute insulin deficiency. B. Epidemiology Approximately xvi million Americans have diabetes, although only slightly more than x million are diagnosed. Type I diabetes accounts for just a minority (about 5-10%) of the cases of diabetes, with an incidence of 30,000 new cases per year. Virtually new cases of Blazon I diabetes occur in patients nether the age of 25 years. Diabetes significantly shortens life expectancy, and one-half of all Type I diabetics dice earlier reaching age l years. The overwhelming majority of diabetics have type Ii diabetes, which has an incidence of 600,000 new cases per year. Type II diabetes is typically diagnosed in individuals over the age of 25 years, with almost half of all new cases occurring in people over age 55 years. Diabetes is especially significant in the Medicare population as more than xviii% of persons over 65 years old accept diabetes. (Just two% of IDDM adults are over 65 years of age.) C. Cost of diabetes The acute and chronic complications of diabetes exert a dramatic toll on both the wellness care arrangement and the morbidity and mortality of diabetes. Diabetes is the seventh leading crusade of death in the United States, contributing to more than 193,000 deaths per year. Diabetic complications include retinopathy, nephropathy, neuropathy, and vascular complications. Diabetes is the leading cause of blindness, stop stage renal affliction, and not-trauma related lower extremity amputations. Additionally, diabetics have a two to four-fold increased risk of cardiac disease and stroke than non-diabetics. It is estimated that diabetes is responsible for $96 billion in direct medical costs and lost productivity each year. The long-term complications are the largest price-commuter. Diabetics spend about 24 million days in the infirmary each year and it is estimated that at to the lowest degree vii one thousand thousand of these hospital days are necessitated by diabetic complications. For instance, Type I diabetics are prone to develop diabetic ketoacidosis (DKA), a potentially fatal pinnacle of claret sugar, which accounts for 3% of all hospital discharges. Both blazon I and blazon II diabetics are predisposed to develop hypoglycemia, which results in xxx,000 hospitalizations per yr. Numerous authors employ the terms "conventional therapy" and "intensive therapy" with dissimilar meanings. This memo will define conventional therapy for type I diabetes as one or 2 subcutaneous insulin injections per day. It volition ascertain intensive therapy as treatment aimed at achieving equally close to normoglycemia as possible accomplished either past iii or more than daily insulin injections or continuous subcutaneous insulin infusion. A. Conventional Handling Management of diabetes involves efforts to maintain blood glucose levels nearly the normal range. Since the discovery of insulin in the 1920s, insulin replacement has served every bit the cornerstone of treatment for blazon I diabetics. Treatment for type II diabetes is somewhat more varied. Some type 2 diabetics achieve adequate glucose control with measures short of insulin replacement (e.g. diet, exercise, oral medications). A major component of diabetes handling involves controlled nutrition and exercise. Exercise facilitates glycemic command in two ways: in the short term exercise decreases firsthand insulin requirements, and in the long term do combats obesity induced insulin resistance by promoting weight loss, especially important for the nearly 40% of Type Two diabetics who are overweight. Many type Two diabetics utilise oral medications (eastward.g. sulfonlyureas) to either stimulate the pancreas to secrete more insulin, or to decrease peripheral resistance. Under conventional therapy, insulin replacement has been provided with subcutaneous injections of insulin one time or twice each twenty-four hour period. For nigh patients, this treatment by subcutaneous injections involves some combination of brusque interim regular insulin and other longer interim insulin preparations. Such dosing as well requires frequent monitoring of blood glucose levels, usually by finger-stick. B. Intensive Command Within the by few years, "intensive therapy" for diabetes management has gained favor as it seems to offer the greatest hope of preventing diabetic complications. Intensive therapy refers to frequent delivery of exogenous insulin (usually by injection four times a day or alternatively by continuous infusion) to obtain tight control in the normal blood glucose range. The Diabetes Control and Complications Trial (DCCT)2, offered compelling bear witness that intensive treatment achieving tight glycemic control reduces the occurrence of microvascular and neuropathic complications in patients treated before the development of advanced disease. This trial involved 1,441 Type I diabetics at 29 medical centers. On average, patients were followed for an average of 6.five years (range iii-9 years) earlier the written report was terminated. The study's master outcome measure was retinopathy, but it also included data regarding renal, neurologic, cardiovascular, and neuropsychological complications likewise as agin effects from treatment. The DCCT examined two cohorts, a primary prevention cohort with a complication-complimentary disease duration of ane to v years, and a secondary intervention accomplice with a affliction grade of ane to fifteen years, and the initial signs of diabetic complications. Subjects were randomly assigned to the experimental group receiving intensive therapy or the control grouping receiving conventional therapy. Subjects in the experimental groups followed an intensive therapy regimen aimed at achieving as shut to normal claret glucose levels equally possible. Intensive therapy subjects had a choice of ii methods of commitment of exogenous insulin; either via 3 or more daily insulin injections or external pump. [By the cease of the study, 42% of the experimental subjects were using insulin pumps]. Subjects assigned to conventional therapy took one or two subcutaneous insulin injections per day. The study's results showed members of the intensive therapy group to accept statistically significantly less progression of diabetic complications than the conventional therapy group: reduction in nephropathy of 34% and 43% for the master prevention and secondary intervention cohorts respectively; 76% and 54% reduction in retinopathy, 69% and 57% reduction in neuropathy (see Table one). The study found no statistically pregnant differences in quality of life betwixt members of the conventional and intensive therapy groups (based on a questionnaire). The report's results were so convincing of the benefits of intensive therapy that the independent data monitoring committee recommended early on termination of the trial. As the evidence favoring intensive therapy accumulated, investigators could no longer legitimately encourage subjects to remain in the less effective conventional therapy group. Table i : Results of DCCT Retinopathy (progression of retinopathy by 3 or more steps) 76% subtract for intensive therapy (95% CI: 62-85%) 54% decrease for intensive therapy (95% CI: 39-66%) Nephropathy (development of microalbuminuria) 34% decrease for intensive therapy (p=0.04) 43% decrease for intensive therapy (p=0.001) Neuropathy (development of an abnormal neurologic exam) 69% subtract for intensive therapy (p=0.006) 57% decrease for intensive therapy (p<0.001) The DCCT demonstrated that intensive therapy offers numerous advantages over conventional therapy past decreasing the development of many long-term diabetic complications. However, in the short-term, the DCCT suggests that intensive therapy may pose some increased risks over conventional therapy. Subjects in the intensive therapy group experienced approximately triple the incidence of severe hypoglycemia (defined as hypoglycemia requiring assistance from another person) compared to the control group (p<0.001). There was even so, no statistically significant difference between intensive and conventional therapy groups for occurrence of DKA or changes in neuropsychological functioning. The increased risk of hypoglycemia prompted the DCCT authors to recommend caution in starting intensive therapy for patients with a history of severe hypoglycemia or hypoglycemia unawareness. Additionally, the DCCT study population excluded prospective subjects who already had advanced diabetic complications. Given that implementing intensive therapy is not risk-free, the authors caution; "The hazard-benefit ratio with intensive therapy may exist less favorable...in patients with advanced complications." C. Continuous Subcutaneous Insulin Infusion Pump Multiple daily insulin injections represented the only available method of tight glycemic command until the development of continuous subcutaneous insulin infusion (CSII) in the late 1970s. CSII attempts to more closely replicate the normal pattern of secretion of endogenous insulin by supplying insulin at a baseline rate augmented past pre-meal insulin boluses. CSII delivery systems involve a bombardment-powered pump which holds a reservoir of buffered regular insulin. The pump propels insulin from the reservoir through an infusion set into a catheter inserted in the subcutaneous tissue of the abdomen (or alternatively the thigh or hip). The CSII systems do non measure blood glucose levels or automatically adjust insulin delivery rates. For proper effect the CSII user must measure out claret glucose several times per twenty-four hours and program the pump to evangelize an appropriate basal rate and pre-meal boluses of insulin. Currently two companies manufacture insulin pumps: MiniMed Technologies of Sylmar, California and Disetronic Medical Systems of Minneapolis, Minnesota. Potential complications of CSII may result from either the inherent effects of insulin or the method of delivery. The most frequent complication involves infection at the infusion site. Pump users generally leave infusion sets in place in subcutaneous tissue for 1 to 3 days, and equally with whatsoever indwelling strange substance, this may precipitate infection. Nearly infusion site infections do non progress across cellulitis although abscesses sometimes develop. The responsible organism is usually staphylococcus aureus and infection is especially prevalent in pump users who are carriers of this bacteria. Less frequent but more serious complications of CSII involve excessive or insufficient delivery of insulin resulting in hypoglycemia or hyperglycemia respectively. Insulin imbalances may occur with all means of insulin commitment including standard subcutaneous injection only CSII introduces some unique mechanisms by which inappropriate insulin dosing may occur unbeknownst to the pump user. In CSII mechanisms the syringe holding the insulin may become blocked, the infusion set dislodged, or the pump otherwise cease functioning without the pump user'due south cognition, causing inadequate insulin delivery potentially leading to hyperglycemia and near-dangerously diabetic ketoacidosis (DKA). Alternatively, incorrect programming of the pump or inherent pump malfunction (sometimes called "pump runaway") may cause excessive insulin delivery resulting in hypoglycemia. Hypoglycemia severe enough to crusade impaired cerebral function may occur with all types of insulin therapy and is estimated to affect up to 30% of blazon I diabetics. The pump devices employ some alarm mechanisms to aid users identify when they are not receiving the intended amount of insulin simply pump users must primarily rely on frequent claret glucose monitoring and subjective symptoms to determine when hypoglycemia or hyperglycemia necessitate aligning of insulin infusion or immediate glucose ingestion. Diabetes direction has been discussed in the Coverage and Analysis Group at HCFA for some time. HCFA has strived to ensure that beneficiaries with diabetes have access to quality care. Most recently, the Balanced Budget Human action of 1997 (BBA '97) expanded benefits to patients with diabetes. BBA '97 allowed coverage of glucose monitors and test strips for Blazon II diabetics every bit well as expanded the types of diabetes education programs eligible for Medicare reimbursement Patient cocky management plays a critical role in the successful handling of diabetes. Traditionally Medicare has paid for some but non all of the tools required for self direction (come across Table two ). Medicare benefits include glucometers, lancets, and glucose examination strips. Medicare benefits currently do not include insulin or the syringes, jet injectors, pen-type injectors, or pumps used to evangelize insulin. Patients employing a subcutaneous insulin infusion pump require somewhat different tools for cocky management than practitioners of multiple daily injections (MDI) or conventional therapy. Like MDI and conventional therapy adherents, pump users would crave glucometers, lancets, and glucose examination strips. Pump users would also require insulin, however, it is either regular or short-acting insulin. Often, such patients require less insulin to manage their diabetes. Most significantly, instead of insulin syringes (except for a few support syringes to use in case of pump failure), pump users would require an insulin pump, (which manufacturers approximate to concluding seven years), and certain disposable supplies necessary for pump functioning including insulin reservoirs, infusion sets, sterile adhesive dressings, and batteries. Tabular array 2: Supplies used in diabetes treatment past conventional therapy, MDI, or CSII Lancets Yes, upwardly to 1 or 2 per day Yes, 3 or more than per day Yes, 4 or more than per day Yes, under DME supplies Glucose exam strips Yes, 1 or 2 per day Yes, three or more per day Yes 4 or more per solar day Aye, express to three per 24-hour intervaliii Glucometer Yes Yes Yes Yes Insulin Yes, regular and other longer interim preparations, unit requirements vary Yes, regular and other longer interim preparations, unit requirements vary Yes, regular insulin, unit requirements vary No Insulin syringes Yes, 1 or 2 per twenty-four hour period Yes, iii or more than per solar day No (except for fill-in) No Insulin infusion pump No No Yes, ane pump estimated to last 7 years (some users keep an auxiliary pump for backup) No Insulin reservoirs No No Yeah, one reservoir every iv.5 days No Infusion sets No No Yeah, one gear up every 3 days No Batteries No No Yep, ane set every 6 weeks No Sterile agglutinative dressings No No Yeah, sufficient quantity to replace dressing every 3 days No The difference in supplies results in different costs for CSII vs multiple daily injections. Based on a cost guess provided by Minimed and analyzed by HCFA staff, the annual toll for insulin pump therapy is approximately $3,329 (judge includes amortized cost of pump over 7 years, pump supplies, insulin, and glucose test strips), vs the almanac cost for MDI $one,817 (estimate includes syringes, glucose test strips, and insulin). The pump itself is the largest commuter of the cost differential; greater market competition, however, would probable bring down the costs of the device. Subcutaneous insulin infusion pumps fall under the do good category of durable medical equipment (DME). Medicare coverage for most external drug infusion pumps is left to carrier discretion, however, regional carriers are currently explicitly prohibited from roofing infusion pumps for insulin. Coverage Issues Manual Department threescore-14 states "An external infusion pump and related drugs and supplies will be denied every bit not medically necessary in the home setting in the post-obit situations: Insulin for the handling of diabetes mellitus." This specific national noncoverage policy has been in effect since 1985. In 1991, the Agency for Health Care Policy and Inquiry (AHCPR) issued an assessment of insulin pump therapy.four The AHCPR assessment stated that "the overall clinical show indicates that CSII is as effective as MDI in attaining normoglycemia in patients with insulin dependent diabetes mellitus who crave intensive insulin therapy." In addition, the written report noted: "Results from a number of controlled clinical trials have shown that CSII devices are effective in providing most-normo-glycemia and in improving metabolic control in patients with IDDM in that location is equally yet no evidence to testify that CSII is superior in clinical efficacy to MDI." AHCPR cautioned that "any form of intensive insulin therapy is likewise contraindicated for individuals with hypoglycemia unawareness and those with untreated preproliferative or proliferative retinopathy." Although the written report noted that CSII poses risks of DKA, hypoglycemia, and skin infections, AHCPR suggested that these risks might be ameliorated as the technology improves. In October, 1994 ECRI, a engineering science cess firm based in Plymouth Coming together, PA, completed an assessment of CSII pumps.5 ECRI concluded that (1) insulin pump therapy produces greater metabolic control than conventional therapy (ii) insulin pump therapy may produce greater metabolic command than intensive injection therapy. (iii) the success of insulin pump therapy depends heavily upon proper patient selection, which in plow, depends heavily upon patient motivation. Regarding risks of astringent hypoglycemic events, ECRI suggested that CSII might offer a decreased take chances compared to MDI but that this is unproven "even though it seems that fewer astringent hypoglycemic episodes are observed during insulin pump therapy than during intensive injection therapy, it would seem clinically prudent to presume that the number of these episodes in these 2 treatment types is equal." Of notation, ECRI recommended circumspection in starting pump therapy on elderly patients considering they may have difficulty responding to the alarm symptoms of hypoglycemia. HCFA reconsidered its position based on new data equally well as the AHCPR and ECRI reports. Reconsideration of the issue of coverage for insulin pumps was raised at the Applied science Advisory Committee (TAC) meetings of March 26-27, 1996, and Baronial 6-7, 1996. At the March meeting the TAC discussed CSII and concluded that "there is no justification for coverage of this service." The TAC further decided that CSII lacked clinical evidence of effectiveness and could non exist classified in a coverable benefit category and as such deemed issuance of a national policy unnecessary. CSII was further discussed at the August coming together and the TAC expressed concern that CSII poses potential dangers while its potential benefits have non been proven for the Medicare population. The TAC concluded that "the scientific data were non sufficient to demonstrate that the infusion pump could provide an effective administration of insulin to any patient in (the) Medicare or not-Medicare population." Currently 153 individual insurers and all but iii state supplemental insurance organizations provide some coverage for CSII. HCFA staff met with representatives of MiniMed in Jump, 1999 to discuss afterthought of the national noncoverage policy for CSII. In May, 1999 MiniMed sent materials which they believed supported a positive national coverage decision. MiniMed provided HCFA with a binder of materials dated May 7, 1999. This binder contained articles from the medical literature which are listed in Appendix B. The folder also contained letters supporting Medicare coverage of CSII, testimonials from satisfied pump users, and a listing of individual insurers and state supplemental insurance organizations currently roofing CSII. HCFA staff supplemented the information provided by MiniMed past independently conducting an all-encompassing literature review. Full cites for the additional studies found are listed in Appendix B. HCFA'due south analysis of the studies provided by MiniMed or generated by HCFA is located in Appendix A. HCFA too reviewed the 1994 ECRI report on the CSII pump as well every bit the 1991 AHCPR report. HCFA engaged in pregnant dialogue with MiniMed as well as their consultants, Patton Boggs, LLP. This dialogue included written, verbal, and face up-to face meetings. Also, communicated with Disetronic Medical System. On July seven, 1999 HCFA sent a letter to MiniMed with a serial of questions relating to the literature. MiniMed responded with a letter of the alphabet dated July 23, 1999. MiniMed's letter included responses to HCFA's questions besides as additional articles from the medical literature. These articles are listed in Appendix B. On August 12, 1999 HCFA met with representatives of the American Diabetes Clan (ADA) and on August 19, 1999 met with representatives of the American Association of Clinical Endocrinologists to substitution scientific information regarding subcutaneous insulin infusion therapy. In reconsidering the national noncoverage policy for subcutaneous insulin infusion pumps, the following questions arise: Analysis of Scientific Information on CSII for Type I Diabetes six Equally mentioned earlier in the text of this Decision of Record, DCCT offers compelling prove that intensive insulin therapy is constructive for the direction of diabetes. As Table I shows, the clinical benefits of decreased incidence/progression of retinopathy, nephropathy, and neuropathy tin can be seen in both the primary prevention and secondary prevention groups. Clearly, intensive insulin therapy is a goal for Blazon I diabetics. The most common method of intensive insulin therapy is a multi-dose regimen of three or more daily insulin injections. Still, continuous subcutaneous insulin infusion pumps are another method of achieving euglycemia. Is it an effective method? Numerous studies, including DCCT, document that CSII is an constructive method of intensive insulin therapy. It lowers glycosylated hemoglobin and decreases incidence/progression of diabetic complications. The question invariably arises equally to how does CSII compare to MDI as a method of intensive insulin therapy? The DCCT offered strong testify establishing the benefits of intensive therapy over conventional therapy, but but limited scientific information exists comparison the two methods of achieving intensive therapy, CSII and MDI. In the DCCT publications, for most consequence measures users of CSII and MDI were reported together, comprising the intensive therapy group, confounding attempts to compare the risks and benefits of CSII to MDI. The DCCT authors notation the fact that intensive therapy patients were non randomly assigned to MDI or CSII and subjects could switch from one method of intensive therapy to the other implies that comparisons of the ii outcomes for users of either grouping "will reflect patient, clinic, and treatment team differences also equally differences between the treatments themselves." Despite the preceding caveat, the DCCT does provide some valuable outcome measures to distinguish betwixt CSII and MDI (see Tabular array 3). Users of CSII accomplished somewhat lower average levels of HbA1c indicating better glycemic control. Although the reported lower values for hateful HbA1c levels practice non independently demonstrate a clinical benefit of CSII, there is some evidence to suggest that any reduction in HbA1c offers some boosted protection from developing diabetic complications. "Although the magnitude of the absolute risk reduction declines with continuing proportional reductions in HbA1c, there are nevertheless meaningful further reductions in risk equally the HbA1c is reduced towards the normal range." This concept is often expressed past suggesting that there is no glycemic threshold for the development of long-term diabetic complications; meaning the goal for diabetes treatment should be to obtain every bit close to normal blood glucose levels every bit possible. Some other surface area where CSII may offer additional benefit over multiple daily injections is for those diabetics exhibiting "dawn phenomenon." Dawn phenomenon represents early morning hyperglycemia idea to result from bereft nocturnal insulin. A report by Koivisto suggests that for diabetics using CSII, the dawn phenomenon may exist prevented by programming the pump to increase the nocturnal rate of insulin infusion. Although niggling scientific data currently exists to show the benefit of decreased early morning hyperglycemia, current beliefs regarding tight glycemic control advise benefit of abstention of hyperglycemia at any time. In a report conducted by Bode et al on patients who had been on MDI and experienced poor glycemic control including severe hypoglycemia, the authors institute that when patients switched to CSII, in that location were statistically significantly fewer episodes of severe hypoglycemia, and no deviation in events of DKA. Of note, HbA1c was not different between the groups, in contrast to other studies which have documented decreased HbA1c for patients on CSII. Tabular array three : DCCT results specific for MDI and CSII Catheter infections NA 7.3 - eleven.3 events per 100 patient years NA Mean HbA1c 7.0% 6.8% Lower for CSII (p<0.05) Hypoglycemic events requiring assistance (per 100 patient years) 44 54 Difference not statistically significant Hypoglycemic events resulting in coma or seizure (per 100 patient years) 10 18 Higher for CSII than MDI (p=0.009) Episodes of DKA (per 100 patient years) 0.8 1.8 Higher for CSII than MDI (p=0.045) A criticism of these studies relating to Medicare coverage, has been that DCCT as well equally the majority of other studies, excluded elderly patients. Although studies on the Medicare population are not an accented prerequisite to coverage, such studies do provide of import information, since the Medicare population is often sicker, with significantly more than co-morbidities than the non-Medicare population. In addition, the pathophysiology of disease is not always the same. Relating to the CSII pump, one must first realize that approximately 5,000,000 Medicare beneficiaries are below the historic period of 65 years (persons with disability and ESRD patients). Some of the beneficiaries could benefit from CSII. More chiefly, the pathophysiology of diabetes is well-known. Although complications are often the result of length of diabetes , the nature of the disease itself does not change as people historic period significant that Type I diabetes is not different pathophysiologically betwixt immature and former adults. In addition, there is a pregnant trunk of clinical experience documenting success for many elderly patients using the pump. At that place are a number of Type I diabetics less than 65 years of age who are doing quite well on the pump. The fact that they turn 65 years of age does not change the nature of their affliction, nor their potential success using the pump. HCFA recognizes that many of the Medicare beneficiaries with blazon I diabetes are likely to have more advanced diabetic complications than the populations studied. However, based on the consistency of the study results demonstrating do good from any boosted reductions in hyperglycemia in type I diabetics, it seems reasonable to extrapolate the data from the available studies to suggest a do good of tight control in Medicare beneficiaries as well. The available studies comparing CSII to other means of obtaining tight control are limited, merely some studies do propose that CSII tin can offer tighter glycemic command than multiple daily subcutaneous insulin injections. There has been some discussion about increased incidence of hypoglycemic unawareness in the elderly. Initially, several authors expressed concern that tight command would predispose patients to hypoglycemia. For those patients who had decreased awareness to hypoglycemia, either because of decreased autonomic response due to previous iatrogenic hypoglycemia or age, failure to accept cosmetic action may cause such hypoglycemia to be life-threatening. CSII may really decrease the frequency of hypoglycemic events compared to MDI. The pharmacokinetics of insulin delivery via CSII differs somewhat from subcutaneous injection. Subcutaneous insulin depots practice non accumulate with CSII. Theoretically, this may diminish the chance of hypoglycemia by eliminating the phenomenon of sudden mobilization of accumulated insulin by such activities as exercise or other deportment that increase claret flow. Recent studies, as well have not substantiated before authors concerns regarding the apply of CSII in patients with a history of hypoglycemia unawareness. In a study on patients with longstanding diabetes and a history of hypoglycemic unawareness, Cranston and others demonstrated that unawareness is reversible. Similar results were obtained in a study by Dagogo-Jack as well equally Hirsch and Farkas-Hirsch. Physicians should exercise caution when they initiate an intensive insulin regimen in patients with a history of hypoglycemic unawareness, but it should non exist a contraindication to the utilize of CSII. Within contempo years, several authors take proposed hypoglycemic unawareness as an indication for CSII. Theoretically, the absence of an insulin depot may crusade delivery of insulin via CSII to exert greater risk of ketoacidosis than conventional injections, simply farther studies are required before it can be asserted that this occurs in practice. In the process of making this coverage decision, HCFA considered the positions of various groups with expertise in the field of diabetes. Several organizations have endorsed the utilise of CSII every bit a safe and effective ways of obtaining tight glycemic command. American Diabetes Clan (ADA) Position: The American Diabetes Association (ADA) is a non-turn a profit arrangement primarily comprised of health care providers and researchers in the field of diabetes besides every bit people with diabetes. The ADA maintains a series of Clinical Practice Recommendations which are developed by experts based on scientific references and are subjected to annual peer review. The ADA endorses CSII in a electric current practice recommendation which states "Both CSII and multiple daily insulin injection therapy are effective ways of implementing diabetes management with the goal of achieving near-normal levels of blood glucose ..... pump therapy is as safe as multiple-injection therapy when recommended procedures are followed."7 The ADA do recommendation did not outline specific criteria for which patients are likely to do good from CSII but it did note the effective use of CSII requires a motivated patient and may be too demanding for some patients. The ADA recommendation farther noted that "in many people, CSII or multiple insulin injections tin can provide equivalent improvements in control" and explained that some clinicians just recommend CSII for patients for whom euglycemia has remained elusive on MDI while other clinicians offer CSII to patients without demonstrated failure of MDI but for whom conventional therapy is not commensurate with their lifestyle. The ADA neither endorsed nor disparaged either of these competing pick paradigms. HCFA discussed this clinical practice recommendation with several representatives of the ADA at a meeting on Baronial eleven, 1999. The published practice recommendation did not specifically address whether the recommendation was for type I or blazon II diabetics, however, the referenced citations were studies conducted on blazon I diabetics. At the August eleven coming together the ADA acknowledged the dearth of evidence for CSII in type II diabetics and expressed its opinion that insulin infusion pump therapy would exist reasonable for type I diabetics in the Medicare population. American Association of Diabetes Educators (AADE) Position: The American Association of Diabetes Educators (AADE) is a non-profit arrangement comprised of wellness intendance providers in the field of diabetes, primarily those involved in diabetes education. The AADE besides published an official arrangement position regarding insulin pump therapy.8 The AADE position statement asserts "given the results of the DCCT, CSII should exist considered a handling choice because information technology offers increased lifestyle flexibility and enhanced self-management that improves claret glucose control. CSII is appropriate for individuals who (1) crave or desire improved blood glucose control, especially during pregnancy; and/or (2) require the flexibility that CSII offers." The AADE position statement comments that hypoglycemia is a business organisation with CSII but frequent blood glucose monitoring tin can aid avert this problem. Like the ADA recommendation, the AADE position statement does not specifically address whether information technology refers to type I or type II diabetics but the references upon which it primarily relies involved studies on subjects with blazon I diabetes. CSII is widely accepted in the medical community. Every bit mentioned earlier, over 150 private insurers presently comprehend this device, including Kaiser-Permanente, Blue Cross Blue Shield, Prudential, and Aetna-US Healthcare. Analysis of Scientific Data on Tight Glycemic Control and CSII for Type II Diabetes The preceding scientific give-and-take focused on Type I diabetes. There are some studies which have tried to affirm that tight glycemic control may help foreclose the progression of diabetic complications in type II diabetics. Some studies of type II diabetes have compared "intensive" handling with "conventional" handling, but the terms reflected much different therapy than how they are usually used in blazon I. For example one study (UKPDS Lancet, 1998) constitute intensive treatment of type Two diabetes to decrease the risk of microvascular but non macrovascular complications, and increase the gamble of hypoglycemia. Even so, where in most of the type I studies, conventional handling entailed insulin injections once or twice each solar day and intensive treatment entailed CSII or insulin injections three or more times each mean solar day, in the UKPDS report on newly diagnosed type Ii diabetics, conventional treatment involved only diet control and intensive handling involved use of a sulfonylurea or any injected insulin. The study found that the intensive therapy group achieved lower mean HbA1c (vii%) than the conventional therapy group (HbA1c seven.9%). The relevance of this written report to the CSII coverage consequence is minimal. In a study conducted in Japan past Ohkubo et al on insulin-requiring type II diabetics, the authors institute a divergence in the incidence and progression of diabetic complications for those patients on intensive insulin treatment. Nevertheless, the number of patients studied was small and no patients with advanced complications were included. In addition, no patients were on CSII. Of note, the authors state that "the benefit of intensive insulin therapy for Type 2 diabetics with advanced microvascular complications is not yet established." The benefits of tight control in full general or tight command employing CSII take non been proven for persons with type II diabetes. Both the body of scientific literature as well as clinical feel demonstrate that more research is needed for Type II diabetes (including insulin-requiring Blazon II): "It is not certain whether the findings from the DCCT regarding intensive insulin treatment for the control of hyperglycemia to prevent complications tin be extrapolated to people with NIDDM... the risks and benefits of reduction of hyperglycemia in people with NIDDM need to be studied in a clinical trial before recommendations tin be made.... While the current epidemiological information suggest that glycemic command is advantageous in people with NIDDM, care should be taken in using intensive insulin therapy to reach such control, because the relation of the risks and benefits of such treatment is not known".9 Given the differences in disease physiology between blazon I and type II diabetes, proof of safety and efficacy for use of CSII for type Two diabetics must be independently established in populations suffering from that illness, not extrapolated from studies of type I diabetics. In determination, HCFA's analysis of the data suggests that CSII is a reasonable and necessary treatment of type I diabetes. Coverage for CSII should exist limited to patients for whom the benefits are likely to outweigh the risks. The coverage policy would limit CSII to patients who have demonstrated ability to consistently and accurately monitor claret glucose at least three times per day and adjust insulin dosing accordingly. Coverage for CSII would also be limited to those patients who accept a glycosylated hemoglobin > vii% at least 3 months prior to starting CSII.Coverage would go on to exist denied for insulin-requiring Type 2. As more data becomes bachelor for those groups, HCFA will revisit the use of CSII for groups other than Type I diabetics. Rescind the national noncoverage policy for external continuous subcutaneous insulin infusion pumps. Meliorate Coverage Issues Manual 60-14 to add: An external infusion pump and related drugs/supplies will be covered as medically necessary in the home setting in the following state of affairs: Handling of Blazon I diabetes. In guild to exist covered, patients must meet benchmark A or B: (A) The patient has completed a comprehensive diabetes education programme, and has been on a program of multiple daily injections of insulin (i.e. at least 3 injections per twenty-four hour period), with frequent cocky-adjustments of insulin dose for at to the lowest degree vi months prior to initiation of the insulin pump, and has documented frequency of glucose self-testing an boilerplate of at to the lowest degree four times per mean solar day during the 2 months prior to initiation of the insulin pump, and meets ane or more of the post-obit criteria while on the multiple daily injection regimen: (1) Glycosylated hemoglobin level(HbAlc) > seven.0 % (B) The patient with Type I diabetes has been on a pump prior to enrollment in Medicare and has documented frequency of glucose self-testing an average of at least 4 times per day during the month prior to Medicare enrollment. Blazon I diabetes needs to exist documented by a C-peptide level < 0.v Connected coverage of the insulin pump would require that the patient has been seen and evaluated by the treating physician at least every 3 months. The pump must be ordered by and follow-upwards care of the patient must be managed by a dr. who manages multiple patients with CSII and who works closely with a team including nurses, diabetic educators, and dietitians who are knowledgeable in the utilize of CSII. Subcutaneous insulin infusion pumps will go along to exist denied every bit not medically necessary and reasonable for all Blazon II diabetics including insulin-requiring Blazon II diabetics. 1 Many people commonly, but mistakenly, label type Ii diabetics who use insulin as having insulin dependent diabetes. Such a characterization is a misnomer, since the physiology of the disease for such patients is different. Type Two diabetics who utilise insulin will be referred to in this text as insulin-requiring Type Two diabetics. 2 The Diabetes Control and Complications Trial Research Grouping published a serial of articles including: "The consequence of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus". New England Journal of Medicine 329:977-986, 1993; "Implementation of treatment protocols in the diabetes command and complications trial", Diabetes Care 18:361-376, 1995; "Resource utilization and costs of intendance in the diabetes control and complications trial", Diabetes Care 18:1468-1478, 1995; "Lifetime benefits and costs of intensive therapy equally expert in the diabetes control and complications trial", JAMA 276:1409-1415, 1996. "The absence of a glycemic threshold for the evolution of long-term complications: the perspective of the diabetes command and complications trial", Diabetes 45:1289-1298, 1996. 3 Exceptions to the 3 per day limit may be granted upon proof of medical necessity and reasonableness. 4 AHCPR, "Reassessment of external insulin infusion pumps", DHHS publication No. AHCPR 91-0030. 5 ECRI, "Continuous subcutaneous insulin infusion pump therapy for diabetes", October, 1994. vi Appendix A gives an overview of all manufactures reviewed. 7 American Diabetes Association, "Continuous Subcutaneous Insulin Infusion", Diabetes Care 22: Supp 1, pg s87, 1999. viii "AADE position argument: education for continuous subcutaneous insulin infusion pump users", Diabetes Educator, 23:397-398, 1999. nine Klein R, "Hyperglycemia and microvascular and macrovascular illness in diabetes", Diabetes Care, Vol. eighteen, No. 2, Feb 1995, pg. 258-268, pg. 265.To: File: CAG-00041N Continuous Subcutaneous Insulin Infusion Pumps (CSII) From: Grant P. Bagley, Physician, JD Managing director Coverage and Analysis Group John J. Whyte, MD, MPH Julie Chiliad. Taitsman, MD, JD Medical Officers Coverage and Analysis Grouping Subject area: National Coverage Decision Appointment: Baronial 26, 1999
Clarification of Diabetes
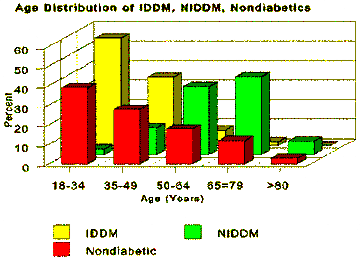
Diabetes Treatment
Upshot Measured Difference Between Conventional Therapy Grouping and Intensive Therapy Group: Principal Prevention Cohort Difference Between Conventional Therapy Group and Intensive Therapy Group: Secondary Intervention Cohort History of Coverage Process
Supply Detail Needed for conventional therapy? Needed for MDI? Needed for CSII? Current Medicare Coverage? Recent Developments and Timeline of Activities
Issues Related to Coverage of CSII
Result MDI CSII CSII vs. MDI
(no p value given) Opinions of Organizations Outside of HCFA
Conclusion:
(two) History of recurring hypoglycemia
(3) Broad fluctuations in claret glucose earlier mealtime
(4) Dawn phenomenon with fasting blood sugars frequently exceeding 200 mg/dl
(5) History of severe glycemic excursions
What Does Level 5 Services Mean Csii?,
Source: https://www.cms.gov/medicare-coverage-database/view/ncacal-decision-memo.aspx?proposed=N&NCAId=40
Posted by: conradforearephe.blogspot.com


0 Response to "What Does Level 5 Services Mean Csii?"
Post a Comment